


Well, it's been a little over three years since we published the first issue of PCNR. Much has changed in nursing and the NHS since then. So as we say goodbye to PCNR in this format, you'll be pleased to know that we will continue to keep you abreast of nursing and health service isssues and clinical developments through our Facebook pages and Twitter feed.

One in three of use will get cancer. Not a good statistic. So we look at ways of preventing it and take advantage of screening where we can.
For we ladies, that means three-yearly mamograms once we get to a certain age. But what if a mammogram isn't good enough? For those with dense breast tissue, tumours are often hidden so go unnoticed until it is too late.
Here, Cheryl Cruwys explains what dense breast tissue is and shares her experience.

You've done it again! Not content with merely trying to deliver a service in the face of swingeing cuts, more patients and less staff, you've been innovating, creating and generally making life easier for your patients.
So in what looks like becoming the annual 'must be there' event, awards were presented to those of you whom your peers had decided were worth a prize!
In issue 13, we presented some of the winners' stories. Here we present the rest.

Social prescribing is really a thing! Initially dismissed as a construct for those patients no-one knew what to do with, the benefits are begining to show.
Whether it's swimming or a language class, simple options can reap amazing health outcomes.
In this article, first published on the Health-Care Arena website (https://healthcare-arena.co.uk) and reproduced with kind permission, Dr Dinah Parhams outlines what it is and how it works.

This article, written by Michael Withers and reproduced with kind permission of HealthCare Arena, explores how working with the AfPP, the concent of 'learning from 'never-events' in the operating theatre was introduced.

As health care professionals, most of us use a little black humour to help us through the tough, horrrific or emotional moments. And we sometimes feel a little guilty about that. So it's reassuring to know that those we care for can also find some humour in their darkest hours.
Given that Mark Pritchard and his wife Sarah had the metaphorical book thrown at them health-wise when Mark had a brain haemorrhage and Sarah developed breast cancer, you'd think that finding a funny side would be akin to finding a Sorbo ring on a pressure ulcer prevention policy, but they did.
A brilliant read!

In previous blogs, shared in PCNR, David has strongly advocated for meaningful patient engagement and his role as a patient Director. Here, he blogs about returing to work after a period of 'pationt-hood'.

The first article Joan wrote for us was about the 6Cs (https://pcnr.co.uk/articles/118/care-is-our-business). We had been in a Twitter discussion about the concept; I was 'fairly outraged' of North London, as I felt that this was fundamental to nursing and should not have to be so baldly stated in a document. Joan however, saw it in a completely different way, so I invited him to pen a piece outlining his view*.
Since then, he has contributed to every issue, and has tirelessly tweeted on our behalf. It's been such a pleasure working with him and seeing how he has progressed to being the Roaring Nurse whom we all love.
*I wasn't expecting him to channel his inner 'vonTrapp family' though!

As it's the last issue, I couldn't pass up the opportunity to share my thoughts once more.
With the upcoming General Election, the NHS is on everyone's agenda. And of course, so is the future of nursing...

In Issue 10 we featured some highlights from the 2015 Ig noble Awards for Improbable research. We liked it so much, we decided to do it again!
As the committee says:
The 26th First Annual Ig Nobel Prize Ceremony will introduce ten new Ig Nobel Prize winners. Each has done something that makes people laugh then think.Winners travel to the ceremony, at their own expense, from around the world to receive their prize from a group of genuine, genuinely bemused Nobel Laureates
Picture Credit: Roman Victory. Thanks to Liam Quin for kind permission to reproduce: http://www.fromoldbooks.org

The NHS is going through what some say is a most diffficult time. That may be putting it mildly!
We may have to learn a lesson or two from the Dakota Indians…
As many variations of these pearls of wisdom are available, I cannot credit this particular version to anyone. But I am eternally grateful for the laughs it produced.

Well, it's a little late, but Happy New Year! I trust that you had a great time, working or not, and that Santa did his thing for you.
They say that every experience is a learning experience - which should be good for revalidation purposes - but here, I share an experience which was more than a learning one - it has changed my outlook.
What would you take from it I wonder?
Cover Picture: Frontispiece: When He Comes He will Rule over the Whole World. Thanks to Liam Quinn for kind permission to reproduce http://www.fromoldbooks.org

Hearing about a user's experience 'straight from the horse's mouth' can be hard; after all, none of us would like to think that we haven't quite delivered what the user was expecting, or the care that we delivered was left wanting. And perhaps for many of us, accepting that people with a long-term condition or disability who are managing perfectly at home do not necessarily want to reliquish their independence fully in during an 'illness' episode, is difficult.
But both are important in order to prevent dissonance between user and nurse expectations.
In this article, Simon Stevens shares his thoughts.

You've done it again! Not content with merely trying to deliver a service in the face of swingeing cuts, more patients and less staff, you've been innovating, creating and generally making life easier for your patients.
So in what looks like becoming the annual 'must be there' event, awards were presented to those of you whom your peers had decided were worth a prize!
Here is a selection of the winners - the remaining fabulous people will be featured in the next issue.

Self administration of medicines by inpatients: are we making any progress? This was a question was posed in a 2013 article by a group of physicians. Frank thinks not so much; read what he has to say.

In Issue 7, we featured an article about ovarian cancer (https://pcnr.co.uk/articles/207/ovarian-cancer-what-you-need-to-know)
I adapted and added to this article for the Health-Care Arena website (https://healthcare-arena.co.uk/dying-of-embarrassment-why-young-women-are-developing-ovarian-cancer/). We are reproducing it here, with permission from HC-A, to mark #CervicalCancerPreventionWeek

Sustainability and Tranformation plans are being hailed as the saviour of the NHS. But are they a force for good, or just another cost-cutting exercise? Joan shares his views.

One can't help but notice that A & E departments are bursting. Everyone from the Government to bed managers are runing around trying to find a solution to the problem. But coul this lie in patient solutions? Here, David Gilbert shares his thoughts in his recent blog.
For more of David's thoughts and insights, please go to: https://futurepatientblog.com/about/

Discharge planning. Two words which strike terror into the hearts of us all. Here, Brian shares his thoughts on how it should be approached.

In the last issue, Frank submitted what he (and perhaps us here at PCNR Towers) thought may be his last piece (https://pcnr.co.uk/articles/333/the-expected-is-always-unexpected). He was v.v. poorly.
However, Frank is a Northerner (hailing from my old home town), and therefore by definition, a hard nut to crack. Dead but won't lie down. Proving that you can live (albeit a little shakily!) with deranged bloods, electrolytes and organs.
Here is his thank you to the staff that cared for him.

In the last issue, we featured a piece by Wayne Walker, Freedom to Speak Up (FTSU) guardian and multi-skilled technician at Torbay and South Devon NHS Trust. Wayne has been in the role for a little over a year now, and this piece reflects his experience.
This blog was written for the NHS Employees site ,and PCNR would like to thank them for their kind permission to reproduce it here
http://www.nhsemployers.org/blog/2016/12/now-that-you-are-a-freedom-to-speak-up-guardian

Not only are nurses twice as likely to suffer financial hardship, but they are three times more likely to face domestic abuse than the public. Paul Steiner, Communication Manager at the Cavell Nurses' Trust outlines the action the trust is taking.

Dehydration is probably the biggest single issue in healthcare, and one of the main causes is the lack of easy access to fluids for people with limited mobility. Those recovering or receiving care in hospital, a hospice or at home who are unable to reach, lift, or hold drinks without help are at risk of dehydration.
This article focuses on a solution.

With the number of people with both Type 1 and Type 2 diabetes increasing, new ways of delivering therapy are being explored. Patch pump delivery sustems offer a great deal of freedom and facilitate self-care.
Here, we focus on a new digital patch pump, the Cellnovo system.
Here is the latest news from Northern Ireland

In her last editorial, Deborah was seething about the erosion of the nursing profession by various actions of the Government.
Two and a bit months down the line, is she still spitting tacks?
Cover Picture: A Siege of the Fifteenth Century. Thanks to Liam Quinn for kind permission to reproduce http://www.fromoldbooks.org

ACA Conference and Exhibition 2017
22nd and 23rd May 2017, Belfast Waterfront, Northern Ireland
Following a hugely successful conference in Edinburgh, we are delighted to announce that ACA Annual Conference and Exhibition will be held on the 22nd and 23rd May 2017 at the Belfast Waterfront in Northern Ireland.

It’s that time of year – parents are sending their offspring to university, worrying how said child is going to cope with washing, ironing, cooking and hangovers. What rarely crosses their mind is the possibility of meningitis.
This article, first published on the HealthCare Arena site (https://healthcare-arena.co.uk/ipad-teddy-bear-menacwy-vaccination-university-essentials/) outlines what to look out for and why prevention is so important
In recent years, lymphoedema has come to prominence as a key issue for the NHS.Accelerate CIC, an established specialist lymphoedema provider in Tower Hamlets since 2008, launched a new model for providing Community Lymphoedema Services to patients across Hackney. This is their story.
The concept of skin failure, particluarly at the end-of life, has gained some traction in recent years. Here, Dr Jeffrey Levine MD suggests that it is a clinical syndrome and may be a contributory factor to unavoidable pressure ulceration.
This is an abridged version of an original article: Levine JM. Skin Failure: An Emerging Concept. Journal of the American Medical Directors Association. 2016; 17: 666-669. Available at: http://www.jamda.com/article/S1525-8610(16)30054-8/pdf
This summary article is reproduced with kind permission of Dr Levine
Some see the use of external (non-NHS) providers as a BAD Thing for the NHS. However, in this article, Nic Parkes, Senior Communications Manager for Virgin Care, outlines how after winning the contract to provide community services in Surrey, worked with nurses and GPs to improve care delivery and communication.

In the last issue, we presented the 2019 Molnlycke Wound Academy Scholarship and Award Winners. Here is Kate Cooper's winning entry for the Innovations in Care (Radiotherapy) Award. While we would usually place the winning entries into the Out of the Ordinary section, as this was such a good case study, we wanted to include this in Practice. So we did.

Patient leaders are an asset to healthcare. In this blog, David Gilbert shares his toughts on being a patient leader.
For more of David's thoughts and insights, please go to: https://futurepatientblog.com/about/

Does your organisation care for its carers? Not all do, as evidenced here by Brian.

As regular readers will know, Frank Booth has been informing and entertaining us with his words based on years of expereince as a nurse and a rather poorly patient! However, despite his robust 'you're not going to get me' attitude to his various ailments, and his acceptance that his was a road that wasn't going to end with a miracle cure, his recent experience rather slapped him in the face.
Read about it here....

Another Olympic and Paraolympic Games has ended. We have watched sports we didn't even know existed, and briefly flirted with the idea that running for the bus was adequate training for the 2020 games...
Here, Joan shares his thoughts on healthcare and how we need to embrace the Olympic ideals
This article, reproduced with kind permission of HealthCare Arena, outlines a simple system comprising the PathAguard® Luca® Antimicrobial Leg Ulcer Cleaning Aid and the PathAguard® ABLiS® (Antimicrobial Basin Liner System), which can be used in VLU cleansing.

Given the shortage of nurses in the UK, you'd think that getting a new job would be easy. But often, recruitment processes can be lengthy and bewildering. Using a recruitment agency can offer help and support for both recrtuiter and job seeker.
In this article, Guy Watson explains what an agency can do for you.

In the last issue, we presented the 2016 Molnlycke Wound Academy Scholarship and Award Winners. Here, we take a look at Lauren Thorpe's Scholarship winning entry in more detail.

In the last issue, we presented the 2016 Molnlycke Wound Academy Scholarship and Award Winners. Here, we take a look at the winning entry in the Innovations in care: Pressure Ulcer Care Award. The UHCW NHS Trust Tissue Viability Team, Amy Verdon, Viola Sidambe and Rachel Reece are using a dolll, Sally Sore as an innovative way of teaching and demonstrating pressure ulcer prevention srategies.

October 19th is FabChangeDay (FCD) It is the brainchild of the team at the Academy of Fabulous NHS Staff, facilitating and supporting staff to brag about, implement or just 'do' big, things that will make a difference to their patients or ways of working.
What will you be doing?

The appointment of a National Guardian for the NHS and local Freedom to Speak Up (FTSU) Guardians was recommended by Sir Robert Francis, following his review and subsequent report into the failings at Mid-Staffordshire.
Wayne Walker, Freedom to Speak Up (FTSU) guardian and multi-skilled technician at Torbay and South Devon NHS Trust, describes his experience in the guardian role.
This blog was written for the NHS Employees site ,and PCNR would like to thank them for their kind permission to reproduce it here (http://www.nhsemployers.org/blog/2016/08/my-experience-as-a-freedom-to-speak-up-guardian)

PCNR is offering one lucky nurse a CPD course, free of charge.
In fact, you even receive a small payment for taking the course!

Featured in one of the early issues of Primary Care Nursing Review, we are delighted to report that Neo-slip, a device to help with the application of compression stockings, invented by nurse Neomi Bennett, has won Entrpreneur of the Year at the National Diversiy Awards in Liverpool last month.

Asthma UK attended the 2016 European Respiratory Society conference in September to hear about and influence Asthma research.
Here is the latest news from Northern Ireland

Back, the, straw, broke, that, camel's the...
Rearrange these works to make a well-known phrase and then read why the Editor is outraged of North London....

Diabetes Professional Care 2016, the leading free-to-attend two-day, CPD accredited conference and exhibition returns on 16 & 17 November, at London Olympia.
The show offers healthcare professionals and practitioners the opportunity to update their knowledge of key suppliers, cutting edge technologies and solutions for the future of effective diabetes management, care and prevention.

PCNR is offering one lucky nurse a CPD course, free of charge.
In fact, you even receive a small payment for taking the course!
One of the side effects of breast cancer surgery is limb lymphoedema. However, patients who have undergone breast-sparing surgery but with some lymph-node removal can develop breast oedema, which is less well-known.
This article is a précis of an original article. PCNR would like to thank the publishers for their kind permission to produce this article.
The NHS is facing increasing demands to provide excellent care with fewer resources. This article outlines the authors worked together with a colleague to develop a set of product criteria that they consider wound dressings should meet in order to include on their WMFs.
The work that the authors have undertaken dovetails with the work currently being undertaken on the development of a suggested national wound formulary. Indeed, it has been seen by a member of the working group who is taking it to them for consideration for use in their processes.

According to Diabetes UK, approximately 345,000 people in the UK are living with Type 1 diabetes. This article explore a new diabetes management system, the Cellnovo system, which has the unique ability to monitor and upload information on patient activity, intake, blood glucose and blood glucose variability, and relay this information to the patient or clinician in real time.
In Issue 5 (https://pcnr.co.uk/articles/166/the-whistleblowers-tale), we highlighted the story of Elieen Chubb, one of the so-called Bupa 7 nurses who blew the whistle on poor care.
Since then, Eileen has been tirelessly compaigning for Edna's Law to be introduced. Here, she relates the campaign's progress.

Are the continence services you provide based on guidelines, guidance or best practice? Frank Booth explores semantics and how these affect practice

After returning from a holiday to his home country, Spain, where he sucessfully made the entire country aware of the great things he is achieving in the NHS, Joan shares his thoughts on the future of the NHS post-Brexit.

Brian's back! And of course, he has something to say. Here he considers what the closure of the DH Nursing, Midwifery and Allied Health Professionals Unit would mean for nursing, and urges you to sign the petition:
https://petition.parliament.uk/petitions/132672

Many of shy away from public exercise - after all, gym's are full of tall and toned people in tight lycra who still look impossibly glamorous even while 'glowing' gently. What could possibly be the problem?
So what is different about taking your exercise regimen to the park? Well, lots apparently. Here, George Winter explains.

Mid-May, the King's Road. A restaurant that used to be a garage. A bevvy of short-listed candidates and a posse of guests all on tenterhooks. Who would win?
Yes, it was the Mölnylcke Health Care Wound Academy Scholarship and Awards luncheon. This article, adapted from the Molnlycke Health Care Wound Academy Bulletin (June 2016), outlines the winning entries.
As ever, PCNR will feature the winning entries in more depth in forthcoming issues.

Changing Faces is looking for a new Chief Executive. After founding the charity in 1992, and being at the helm for the last 24 years, James Partridge is standing down. Here, we carry James's article (written for Viewpoint, the charity's newsletter - https://www.changingfaces.org.uk/viewpoint-moving-aside-founders) which reflects his thoughts on setting up CF and why he is leaving.
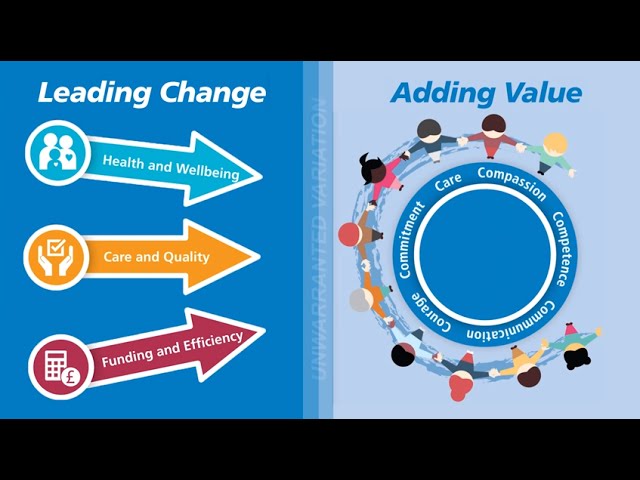
'Compassion in Practice' concluded this year. So what is next? Oh look, another document, Leading Change, Adding Value, which according to Jane Cummings
"...is a framework every nursing, midwifery and care professional, in all settings, can use to ensure that we achieve the best quality of experience for our patients and people, the best health and well-being outcomes for our populations, and use finite resources wisely to get best value for every pound spent".
Here is the executive summary

Rather like pain, leadership is what the individual says it is. We all want different things from a leader, which makes their job that much more difficult. And are the leadership skills required in the private sector the same as those required in the NHS? Are NHS staff particularly clinical staff, inherently good leaders? Do they have to be taught leadership?
Dr Umesh Prabhu, Dr Umesh Prabhu, FRCPBH, Medical Director at the Wrightington Wigan and Leigh Foundation Trust (WWLFT) shares his thoughts.
If it's happening, it's here! If it's not, let us know - PCNR is happy to publish your good news stories or reports on events etc.

Those of us aged over 40 are probably more used to using pen and paper to communicate. However, with age comes a noticable failure in memory - sometimes we are simply too busy to remember appointments, or indeed, to remember to look in our diaries. So a system that can send us reminders via mobile phone can only be a good thing.
Here, Joan Pons-Laplana outlines his experiences with Flo Telehealth.

In the last issue (Issue 9: http://https://pcnr.co.uk/articles/258/oh-what-a-circus-oh-what-a-show-) we reported on the Academy of Fabulous NHS Stuff Awards, held in November last year. We also featured two of the winning entries.
Here, we show-case the other award winners.

In the last issue (Issue 9: http://https://pcnr.co.uk/articles/258/oh-what-a-circus-oh-what-a-show-) we reported on the Academy of Fabulous NHS Stuff Awards, held in November last year. We also featured two of the winning entries.
Here, we show-case the other award winners.

In my recent editorial ‘In, Out, Shake it All About’ (Issue 8: https://pcnr.co.uk/articles/249/in-out-in-out-shake-it-all-about), I postulated that the revalidation process was likely to be a bit unwieldy. On a personal note, as I am self-employed, I was worried about finding someone to have my reflective discussion with and someone to sign off all the paperwork. Fortunately, a colleague came to the rescue and offered to do both jobs (see, a nurse multi-tasking again).
In return, I agreed to write about my experience of revalidation. So here goes…

Unless you have been up in the International Space Station for the past two years, you won't have escaped the bru-haha around 'safe' staffing numbers. First NICE was working on a model, then they weren't, someone else was going to do it...
However, while various organisations, including the DH, were spatting over this, Ann Marie Riley, Caron Swinscoe, and various other innovative people came together to produce a model of staff for their organisation.
Then they made it into an App...

There is data to support the problems of healthcare and hospital acquired infections (HAI) associated with ‘traditional’ hospital basin bathing equipment.
The ABLiS™ antimicrobial basin and liner system provides a cost-effective, practical way of ensuring infection control in hospitals, nursing homes and home environments.

It happens to us all eventually - forgetting what day it is, looking for your car keys and inexplicably finding them in the fridge, conversations with phrases such as 'you know, the thingy...' because you can't quite remember the word for the thingy you are talking about.
Of course, such lapses are not always an indicator of dementia - we all lead busy lives and often are just working on autopilot. But what are the causes of confusion in your patients?
In this article, Sue explains how a few simple steps helped her mother to overcome her confusion.

The Victorians knew how to do a good death. Mourning was almost an art form. Professional mourner was a legitimate career option, bodies were kept at home prior to the funeral, and Queen Victoria made black clothing and retreating to one's country pile de rigeur.
Over the last 150 years or so, society's attitude to death has changed. It's almost a taboo subject.
In this article, Frank Booth explains why we should all be talking about it.

Here at PCNR we know an innovation when we see one! There are those that are ground-breaking and make headline news, there are those that make a difference to a few. And there are those that are so simple, yet so reproducible across the entire NHS, you wonder why no-one has thought of it before.
This is one such innovation…

Sometimes you look at the titles of nursing research articles and lose the will to live: for example, 'Instantiating informatics in nursing practice for inegrated patient centred holistic models of care: a discussion', or 'A meta-ethnography of the acculturation and socialization experiences of migrant care workers'. That's not to say they aren't interesting once you start reading them of course, but such titles sometimes make you wonder if the journals only accept articles with titles that are at least as long as the research report.
The Ig Nobel Prizes for Improbable Research is a parody of the Nobel Prizes and is given out each year for ten unusual or trivial achievements in scientific research. The stated aim of the prizes is to "honor achievements that first make people laugh, and then make them think". Here are a couple of examples.
Picture Credit: Roman Victory. Thanks to Liam Quin for kind permission to reproduce: http://www.fromoldbooks.org

David's blogs are usually found in our Comment and Opinion section. However, as this blog focuses on his role as a Patient Director - a new and innovative role - we feel it sits well in Out of the Ordinary.
The House of Commons has just released a report on primary care*. Such an important piece of work on the future of General Practice and General Practice Nurses shouldn't go unnoticed. We've summarised the relevant nursing references here.
* House of Commons Health Committee. Primary Care. Fourth Report of Session 2015-16. http://HC 408. http://www.publications.parliament.uk/pa/cm201516/cmselect/cmhealth/408/408.pdf

The latest news from the Queen's Nursing Institute:
‘Nursing for All’ – A national conference about nursing the most vulnerable
Friday 17 June 2016

Mmmm... it's all been a bit bonkers at the DH. Mr J Hunt is certainly not flavour of the month with the junior doctors, and then there's the whole bursary thing.
So what else is in the news?
We seem to be having a bit of a tele-health focu this issue. News of a fabulous event taking place in June - here!
Want to know what RCN NI is doing for you? Read all about it here.
Want to know what RCN Wales is doing for you? Read all about it here.
Want to know what RCN Scotland is doing for you? Read all about it here.
Want to know what RCN England is doing for you? Read about it here.

A new nursing associate role has been proposed. The concept, currently out for comment, aims to encourage more people into nursing and address the 'numbers' crisis.
Deborah shares her thoughts

Negative Pressure Wound Therapy (NPWT) has been used in the managment of open and chronic wounds since the 1970s. And it has been shown to be very effective. But does it have a role in the prevention of incisional wound breakdown?
In this article, first published on the Health Care Arena website (http://www.healthcare-arena.co.uk), and reproduced by kind permission, outlines work in this exciting area.

You've read about the lunch and the winners...
Here, we look at two winner's projects in a bit more depth
The rest will be featured in the next issue

It's here.. yes, social media is now a part of our lives and like it or hate it, it can be a force for change in practice.
In this article, first published on the Health Care Arena website (http://www.healthcare-arena.co.uk), and reproduced by kind permission , outlines work in this exciting area.

You may remember in the last issue of PCNR we carried an article about the dangers of polypharmacy, particularly in the elderly (https://pcnr.co.uk/articles/232/problematic-polypharmacy-the-drugs-don-t-work-they-just-make-you-worse).
In this article, Frank Booth shares his experience and cautions health professionals.

The New Year bought with it some excellent news for our PCNR Editor, Deborah Glover.
She's way too modest to write about it herself so it's up to me your publisher, to do the decent thing. Now all I have to do is spread this far and wide through social media before she deletes it...

For patients, the communications they receive are practically and symbolically important. An appointment letter may be the first time they come into contact with the health service. You'd think therefore that this simple thing would be done corrrectly, every time...
In his latest blog, David Gilbert finds that this isn't the case....

In Issue 4, Brian Booth discussed professional boundaries.
In this follow-up article, he challenges you again...

Are you a fan of Call the Midwife? Sue Smith looks back on childbirth approaches practice in the 60s. And no, it wasn't all Patchouli and free love (although that may be why Sue was delivering some of the babies she delivered...)

Remember back in Issue 6 when we featured the Academy of Fabulous NHS Stuff? Well, there's more...
On 26th November, there was a gathering in Shoreditch (no vaccinations required apparently, although a team from 'oop north were heard to say "£45... for a haircut...???...ee that would never do with us..."). NHS staff (yes, those actually doing some work), voted for their favourite project posted on the Academy wall, and accordingly, the Academy of Fabulous NHS Stuff gave an awards lunch.
And it was fabulous.
Our Editor, Deborah, was an accessory....

Something magical happened this Christmas. A wave of pride in the NHS swept the nation, taking the NHS Choir all the way to the prestigious Christmas number 1 slot. This was something few of us, even in our wildest dreams, thought woud be possible!
For once we made the news headlines for the right reasons, and the front pages of the newspapers where splashed with a simple message: Our love for our NHS!
Joan Pons-Laplana shares how it happened.

Is the NHS on the brink of collapse, going to hell in a handcart or ticking along nicely? It is doubtful that anyone working in the NHS would think the latter option, and most probably agree with the first.
In this article, the first of three commissioned by Healthcare Arena (https://healthcare-arena.co.uk/), Deborah Glover outlined the history of the NHS

The first of these three articles commissioned by Healthcare Arena (https://healthcare-arena.co.uk/) outlined the history of spending on the NHS. In this article, Michael Withers explores how the NHS may (or may not!) be fixed.

In the final article of three commissioned by Healthcare Arena (https://healthcare-arena.co.uk/), Stewart Munroe, owner of Pentland Medical, and Dr Aisling Koning outline where the NHS goes from here.
On the 17th December 2015, the Minister for Health, outlined nursing education reform and a new route into nursing.
This is his statement.

The sun was shining in the East End of London last May. Docklands was somewhat stunned to have over 4000 people from over 70 countries decending upon them to talk about wounds...

“I would advise joining a local Leg Club”, wrote Dr Ellie Cannon for The Mail on Sunday on 17th January. “These are community-based initiatives proven to help patients treat, manage and live with leg ulcers through collective treatments and peer support”
Roland Renyi, Chair of trustees of the Lindsay Leg Club Foundation explains why this national recognition of the Lindsay Leg Club model is so exciting.
Want to know what RCN NI is doing for you? Read all about it here.

All the latest from the NMC. Remember, revalidation is only three months away!

Need to know what's happening at a national level? look no further!
Our resident commentator, Joan Pons-Laplana is doing it all again - running that is. This time, it's for the Cavell Nurse's Trust.
Read about it here and how you can support Joan.

October the 12th of this year marked the 20th World Arthritis Day. Currently, around one in seven people in the UK currently live with arthritis and this figure is expected to rise to one in four in the next 15 years.
This article by Dr Wendy Holden, outines how the charity Arthritis Action helps those with the condition and how you can help your patients who have arthritis.

Exudate management is one of the most challenging aspects of wound care. In this article, Sylvie Hampton outlines why managing exudate is important and how dressings contribute to effective healing.

For most of us, discussing anything to do with our bowels will only happen when hell freezes over. But the state of our stools should be talked about in order to prevent constipation and/or its associated complications.
In this article, Frank Booth outlines prevention and management strategies.
For many patients, particularly the elderly, multiple comorbidity management requires many different drugs. In this article, Dr Aisling Koning outlines the issues of polypharmacy.
This article was first published on the Health-Care Arena website and has been produced by kind permission of Pentland Medical.
This case study, adapted from Rosemary Rose's Molnlycke Wound Academy Scholarship and Awards winning entry, suggests that negative pressure wound therapy (NPWT) and allogeneic keratinocytes can be used successfully as an alternative to a skin graft to heal full thickness skin loss head wounds.

Society's attitude to death today is far different to that of 100 years ago. Granted, it isn't so commonplace anymore - technology, drugs and gizmos keep us alive longer even than our allocated three score years and ten!
As healthcare professionals, we shoudl be used to discussing death, we see it every day. But we are also members of society, so perhaps our attitude has also changed and death is seen as a failure.
Sue Smith explores this fascinating subject

How easy is it, in this fast-paced, short-staffed world of nursing, to remember the names of your patients?
Brian Booth has a few thoughts...

Do leaders and managers ever feel vulnerable? Have you ever sat in a meeting and suddenly thought "Do I really know what I am talking about? Is this me? I don't know what the hell is going on? And if you have, do you tell anyone, or even admit it to yourself?
I his latest blog, David Gilbert shares his thoughts on the vulnerabilities of a patient director.
Developments in both the sophistication and affordability of mobile technologies using custom-designed hardware and software are changing how healthcare is delivered, received and researched. Healthcare workers and pioneers alike are embracing mobile technology, including social media educational tools, mobile apps, wearables and other digital tools.
Here, Dr Aisling Koning outlines potential applications in care.
This article was first published on the Health-Care Arena website and has been produced by kind permission of Pentland Medical.
When you watch Countdown, are you better at the word games or does the maths game make you sqeal with excitement? Ever wondered what happens to all those stats you send to 'the beast'?
Well, Jon Hannah of NHSIQ, reveals all. Jon or a member of his team, will be a regular contributor to PCNR, keeping us up to date with developments and news.

How difficult is it to understand 'foreigners'? Not just the ones from countries where English if not the first language, but those from areas outside of your own - what does the phrase 'Well I'll go to the foot of our stairs mean?
Does it matter if you don't quite get it? Well yes, if you are trying to communicate with your patient.
Here, Joan Pons-Laplana shares his experiences.

Following a hugely successful conference in Brighton, we are delighted to announce that ACA Annual Conference and Exhibition will be held on the 23rd and 24th May 2016 at the Edinburgh International Conference Centre.
The theme of this year's programme is Transitions in Continence Care.
There will also be an extensive exhibition which will feature over 50 companies offering new innovative products and practical solutions.
It's not often nurses and other health care professionals get something for nothing Of course, there's PCNR, which is free, and now there is another site that is a vaulable resource.
We all love a new therapy, especially in the world of wound care. A novel treatment is combined ultrasound and electro-field stiumlation.

Things are moving fast at the NMC. All the latest news is here.

Against a backdrop of a lifetime career as a health care professional working with children and families, Kate H-N has produced six Relax ‘n Learn Teaching Tales, designed to raise and tackle some common issues that affect children’s happiness and which, if left unspoken about and not addressed, can lead to unnecessary unhappiness with mental health problems and behavioural disturbance, which typically attract unhelpful, stigmatising labelling. In this article, Kate outlines how Eric the Oracle can help develop the emotional health of children.


Responsibility for public health nursing and midwifery leadership is based in the Department of Health and Public Health England (PHE). Viv Bennet acts as Director of Nursing and Midwifery and also as the government’s principal advisor on public health nursing.
But do we see PH as important? Is it something nurses readily embrace? It seems not...

Using suction to remove toxins or to stimulate wound perfusion is not new. However, the therapeutic use of mechanical negative pressure for wound management has developed exponentially over the past three decades, with a consequent rise in the number of therapies available. In this article, Sylvie Hampton guides us through the use of negative pressure.

Ovarian cancer is the fifth most common cancer affecting women in the UK, with 7000 new cases diagnosed each year. It is the biggest gynaecological killer, resulting in 4300 deaths annually; this is more than cervical and womb cancer combined.
For women diagnosed in the UK, prognosis is poor - the 5 year survival rate is 43%. To improve survival rates there is the need to improve the recognition of symptoms, understand those who might be at a high risk of developing ovarian cancer and speed up diagnosis and referral to secondary care.
In this article, Ovarian Action, a charity advising and caring for women with ovarian cancer, outlines the important role nurses can play in improving survival rates by raising awareness of the symptoms amongst patients and the general public in the primary care setting, and includes a case study of one woman's experience.

Gout is generally considered to be somewhat of an old-fashioned disease, conjouring up images of crusty and grumpy old colonels with very large bandages on their foot.
Unfortunately, 21st century life-styles and diets have seen it making something of a 'comeback'. In this article, Frank Booth outlines the signs and symptoms and provides a personal view of his experience.

In an effort to force NHS organisations to save money, the Government imposed a cap on agency staff spend. But is this the answer to the problem? Joan-Pons Laplana doesn't think so.

Plus ça change, plus c'est la même chose...
If you stay in nursing long enough, you'll see many changes, and you'll see many things turn full circle. Here, Sue Smith shares her reflections on change.

While many patient groups and organisations exist, it is rare to hear an unbiased view of care from a service user.
We at PCNR are fortunate enough to have such a voice; David Gilbert, currently Patient Director at Sussex MSK Partnership and Director of InHealth Associates, is a former mental health service user with 25 years experience in patient/user and public engagement at local, national and international level.
Over future issues we will include David's blog, and in issue 8, an article from David explaining his role as Patient Director. Here, David outlines 'The Patient's Dozen', 12 issues important to patients and carers.

Are well all getting that little too self-centred? Getting cross when we have to pull over for an ambulance? Angry when 'a passenger is taken ill' on the train, causing a delay? Feeling that although I am a registered nurse, I can't stop to give assistance else I wil be sued...?
In this opinion piece, Brian Booth outlines his personal expereince and poses a question for the reader.

At the end of May, the winners of the Mölnylcke Health Care Wound Academy Scholarship were announced at a luncheon held at the Royal Opera House on the 28th May.
This article, adapted from the Molnlycke Health Care Wound Academy Bulletin (July 2015), outlines the winning entries.

The Spark is an inspiring three hour event hosted by local catalysts for change hosted in a community space for up to 100 people who are passionate about the future of health and social care services.
Joan-Pons Laplana explains more and outlines how you can get involved

Revalidation, due to be implemented in 2016, will affect all Nursing and Midwifery Council (NMC) registrants. Revalidation is the new process by which all nurses and midwives every three years, will declare and demonstrate that they remain fit to practise. As a consequence, it is the most important change to NMC regulation since the introduction of the post-registration education (Prep) standards in 2001. It is an exciting prospect, but some people consider it daunting: it need not be.
In this article, David Foster outlines what it means for you.

To paraphrase Supertramp, ..'it came all the way from America...'
The Transatlantic Trade & Investment Partnership (TTiP) is essentially a planned trade pact currently being negotiated between the European Union (EU) and the United States of America (USA). If it comes to fruition it will become the world’s largest bi-lateral trade agreement.
The central objective of TTiP is to remove regulatory barriers to trade for big business including food safety law, consumer protection standards, environmental legislation and the sovereign powers of individual states.
In this article, Daniel Legg outlines what this means for the NHS
Revalidation for nurses and midwives is achievable, desirable and realistic, according to initial findings from 19 revalidation pilot sites across the UK. More than 2,100 participants from a range of health and social care settings took part in the pilots earlier this year and many felt that revalidation was a positive experience.
(From NMC.org.uk)
Look inside for a round-up of what's happening in Norther Ireland that's pertinant to nuses
'The Queen’s Nursing Institute welcomes the publication of ‘Safely Home’ by Healthwatch England.
(From QNI.org.UK)

Woundcare4heroes charity was founded in 2012 with a mission to bridge the gap of trauma aftercare services to provide lifelong care pathways and a single point of contact for veterans transitioning into our NHS following injury during military service.
Wcare4H have spent almost four years exploring the needs for veteran trauma aftercare services, raising awareness amongst practitioners and the veteran community, developing care and wound prevention pathways, providing clinical services, education and advice to healthcare practitioners, veterans and their families.
People who are in their final days of life in hospital should be assisted to receive hydration, according to a draft guideline from the National Institute for Health and Care Excellence (NICE).
(From RCNi)
The European Medicines Agency has launched a review into the safety of medicines called SGLT2 inhibitors that are used to treat type 2 diabetes.
(From RCNi)
NICE’s latest guideline aims to improve survival rates and reduce variation in the care of patients with melanoma, currently the fastest growing form of cancer.
(From NICE.org.uk)
Outdated treatment, uncertain funding and failure to battle big causes of cancer – with one in five people still smoking – blamed for unnecessary suffering
The National Institute for Health and Care Excellence (NICE) has just published new guidelines aimed at helping to improve employee health and wellbeing. The guidance supports a leadership model which promotes the wellbeing of employees, informed by an understanding of the role corporate culture can play in this

Scottish exhibition organiser, QD Events, are delighted to announce the launch of a new event with the twofold aim of offering advice, support and information for individuals living with disability or a long-term condition, and providing learning, product knowledge and networking opportunities for healthcare professionals in Scotland.

This month's selection of Tweets and other items which caught our attention.
If you have any comments, opinions or would like to submit an article, please email, Tweet us or leave a comment on our Facebook page. We would love to hear from you.

So, it's election time. All parties have made a big bru-haha about the NHS; millions, nay, billions of pounds will be invested ("if we get back in", or if "you elect us"...) I ask, if they can suddenly find all this money, why haven't they been dripping it into the system already?
So I'm not going to talk about this particular bun fight. Open to find what's on my mind...

There cannot be many of you who haven't heard about Dr Kate Granger and her Twitter campaign #hellomynameis. I recently had the pleasure of listening to Kate speak. It was depressing to hear of her experiences. After all, if nurses can't even be bothered to communicate with their patients, what hope is there is instilling confidence?
In this blog, Kate outlines why she started the campaign and what has grown from it.
In September 2014, the Lindsay Leg Club Foundation (LLCF) was awarded a grant by the Department of Health to produce and disseminate a Compendium of Best Practice from within the large network of Leg Clubs currently operating in England. The idea behind the project was to understand, co-ordinate and summarise the best practices undertaken by the volunteers, nurses and members who attend the Leg Clubs every week, and to share that information among Leg Clubs, and the healthcare community at large. This article reports on the outcome.

Exudate management is a challenge in chronic wound healing. Too much will delay healing, as will too little. But how much is too much? Do we fully understand what it does? In this article, Sylvie Hampton provides some answers.

You may remember that we featured Helen Mountford's winning Molnlycke Scholarship entry, in issue 2. Then, in issue 3, we carried an article about Acorns Hospice, Helen's place of work. In this issue, Helen outlines how she and the team have developed a wound care prevention and management programme for children.

In part two of this overview of diabetes, Frank gives a svery simple summary of treatments and shares his experiences of diabetes.

An in-house stop smoking service at King’s Health Partners, targeting NHS staff, has achieved an impressive 60 per cent quit rate at four weeks. Jo Carlowe finds out how they did it.
(Original article published in The Advisor Spring 2015.)

Well, it’s finally here. The Code (2015) became effective from 31st March. Many believe it was sorely needed. Others believe it is just more ‘gumpf’. Yet this version will have more impact upon registrants as revalidation depends on adhering to and demonstrating where you have applied its principles. In this opinion piece, Brian Booth and Deborah Glover share their thoughts about the new Code.

Ian Peate is a Professor. The route to becoming a Professor of anything is not easy; many degree-course Registered nurses do not attain such heights. But Ian began his career as a State Enrolled Nurse - you know, the course that apparently existed for the 'less academic', less motivated' people...
Read his story...

Millions of pounds are spent every year by women (and men!) who want to change some aspect of their appearance. Or they want to look like someone completely different (was M Jackson trying to become Diana Ross - the jury is still out..). Yet many who have facial disfigurements due to genetics, illness or injury are living full and active lives without feeling the need to have aesthetic surgery.
Her, Sue Smith ponders why...

In March, NHS Change Day events took place across the country. In this article, Joan Pons Laplana describes how it can work for you.
Whistle-blowing is the act of reporting a concern about a risk, wrongdoing or illegality at work, in the public interest.
Raising concerns about such poor practice should be the norm, accepted as an important part of people’s day-to-day work, as they reflect on their professional practice and work to improve their service.

With all the negative press about the NHS, you'd be forgiven for thinking that you work in an untenable system that has lost its ability to innovate or care. But actually, you'd be wrong in your assumption. Innovation and teamwork are alive and well! The Academy of Fabulous Stuff, the brainchild of Roy Lilley, Dr Terri Porrett and Jon Wilkes is a repository for, errm..., fabulous NHS stuff!

Post 2008 financial crash, political rhetoric has centred on public sector bodies providing more for less and the NHS has not escaped this mantra. As a consequence, procurement departments have been thrust into the limelight as NHS Trusts search for ways to reduce their non-pay expenditure. Historically procurement has been seen as a transactional back office function; however more recently procurement departments are being relied upon to conjure up new approaches to reduce expenditure. In this article, Daniel Legg outlines his role.

Changing Faces’ ‘Look at Me’ report finds that effective treatment for the psychosocial effects of skin conditions is the exception rather than the rule...
...Changing Faces calls for psychosocial care to be placed on equal footing with physical care with better resourcing of integrated community dermatological services.
All the latest news from the RCN Northern Ireland
The RCN have been busy. Read about what they've been up to here.
Very interesting legislation regarding time to appeal against a Conduct and Competence Committee (CCC) decision.

This month's selection of Tweets and other items which caught our attention.
If you have any comments, opinions or would like to submit an article, please email, Tweet us or leave a comment on our Facebook page. We would love to hear from you.

It is possible to eat, drink and be merry without overdoing it. In this article, Victoria Taylor offers her tips for eating out and/or partying, which help look after your heart and waistline.

It is theorised that nurses are sometimes afraid of compression due to lack of education, inexperience or inability to obtain necessary equipment. Nevertheless, there are simple methods of assessment and use of compression; in this article, Sylvie Hampton will attempt to guide the nurse with less experience in how to assess and use compression safely and with confidence.

Diabetes has a world-wide reach and prevalence is increasing. But how much do we know about it? In this article, the first of two, Frank Booth outlines types and causes of diabetes. In the second article (Issue 6 PCNR), he explores these factors in greater depth and presents his own view of living with diabetes.

The @ProudToNurse Twitter camapign and the #mynameis... and the 6Cs are gaining traction in the nursing and clincian community, with jolly good reason. Here at PCNR we support the philosophy of these actions and are planning to feature updates in each isssue. But behind these are passionate people who generally are unsung. In this article, Maria Davison explains why she is @ProudToNurse

The 6Csy day held at Leicester racecourse last month was an unexpected 7 hours of pure enthusiasm, passion and pride about nursing from nurses. Joan sought to re-ignite the spirit of caring, and succeeded beyond expectation. Here both he and Deborah share their thoughts on the day.

Are you keen to help children develop their resilience, self-esteem and confidence so they can improve their emotional health and well-being and learn some key skills for creating their own happiness? In this article, Kate H-N the author of the Brockley Bank tales, outlines how the adventures of Eric the Oracle can help develop the emotional health of children.

Having come from a background in art (I was a Deputy Director at Sotheby's auction house), I definitely never thought I’d end up becoming an undertaker! Poppy Mardall, founder of Poppy's Funerals believes that the nursing profession has such an important role to play in allowing people to talk openly about dying and what happens after death. In this article, she explains why she moved into the business and how a colourful, personalised funeral can make all the difference to grieving family and friends.

This month's selection of Tweets and other items which caught our attention.
If you have any comments, opinions or would like to submit an article, please email, Tweet us or leave a comment on our Facebook page. We would love to hear from you.
The management of venous leg ulceration can be problematic. Healing ultimately depends on correcting the underlying cause, namely venous incompetence. Debates continue on the most effective approach - compression, which can be a lengthy process and not always clinically appropriate, or surgery or stenting? Naturally, for some patients, surgery is not an option. But are we denying those who may benefit from such an approach? In this challening article, Professor Mark Whitely outlines why he believes that compression should only be an intermediary step.

Should nurses, male or female, have visible tattos? We could argue that one's visible appearance is not necessarily a reflection of ones knowledge, skills or caring ability. But we all have perceptions, as do our patients. Do tattos go against the ethos of our Code, which states we should look and behave as professionals when on or off duty, or is this nonsense as they are an acceptable body mutilation in the 21st century? Brian Booth gives us his thoughts.

If you watch any of the myraid cooking programmes, you'll probably know that presentation of the food is almost as important as taste. There seems to be a fashion in certain pubs and restaurants to serve meals on a roof tile, a wooden board, or a dustbin lid (I may have made that one up...). While we can but shudder at the infection control implications of such platters, are they merely pretentious, or do they help tempt us to eat? In this article, Sue reflects on a lesson learnt about plates....
Despite legislation to support staff and the requirements of our Code, many nurses remain reluctant to report issues of concern such as poor care, staff numbers or bullying. Why? The experiences of Eileen Chubb, outlined here, may hold the answer.

In April this year, NHS England will impose a new national workforce race equality standard on the NHS through the NHS standard to address inequalities in BME representation at all levels in the NHS. Here, Joan Pons-Laplana presnts his thoughts as to why we should all be embracing such standards

Following a hugely successful conference in Birmingham which again was sold out, we are delighted to announce that ACA Annual Conference and Exhibition will be held on the 4th and 5th June 2015 at the Hilton Brighton Metropole.

There is still time to purchase the 2015 QNI Calendar. This year the illustrations are vintage nursing photographs from the early years of the NHS, rediscovered last year in the home of a former District Nurse. They show nurses at work in London and in Norfolk, treating patients of all ages.
A round-up of news and information from RCN Northern Ireland
All the latest from the NMC. Let us know what you think of the way the organisation is working for you: enquiries@pcnr.co.uk

The QNI is delighted to announce their 4th Annual one day Conference in London on Monday 28th September 2015 at the Royal College of General Practitioners, 30 Euston Square, London NW1 2FB.
Is the Cancer Drugs Fund (CDF) just vireing money around, effectively robbing Peter to pay Paul?

The London IPS Branches present: Infection Prevention – Are YOU Ready, Prepared and Equipped??

A focus on the 6Cs

Attending Wounds UK Annual conference at Harrogate? Then don’t miss the Activa Symposium, chaired by Angela Rippon
A large part of neuropsychiatry consists of medicines management. Patients may have been prescribed medicines for signs and symptoms which turn out to have no physical cause. Psychoactive drugs tend to need careful management, so there is often a lengthy process of weaning off one drug whilst introducing new ones (whose dosage needs titrating), all the while monitoring the patient carefully.
Changes in prescriptions may take some time to filter down to the pharmacists, who might continue to dispense repeat prescriptions for a lengthy period before they become aware of any changes. This article outlines how one nurse found a simple answer to this problem.
Incontinence Associated Dermatitis (IAD) is challenging to both identify and manage. The damage associated with IAD occurs when a patient’s skin is exposed for prolonged periods to sweat, urine, faeces and exudate. This article discusses IAD and provides case studies in which a barrier cream has proven effective in the management of these lesions.

The roles of nurses, midwives and care staff have significantly changed in recent years. We have learned new skills and our responsibilities have increased accordingly. This has presented some challenges. This article describes how the 6Cs can help guide staff.

Generally speaking, most clinicians know something about heart failure, even if it’s only the obviousness of the words. Rarely do you have the opportunity to experience catastrophic heart disease and survive to tell the tale. This article, written by a retired nurse and patient, explains in a very personal way, how you can and should make a difference to your patients, and asks you to be confident that you can make a patient’s life better.

This article gives a brief overview of hyperhidrosis, a debilitating condition affecting at least 1% of the population. Any part of the body may be affected, such as the face, head, neck, back or groin; but most commonly the hands, feet and axillae are the primary concern.

The nursing hierarchy in 1979, the year I started nurse training, was awful; but even then, people yearned for the good old days in ways which some readers may accuse me of doing, should they ever get to the end of this article.

Did you sleep well? Tucked up in a cosy bed? Had a nice bath? Smelling sweet?
Such thoughts take me back fifty years to working in Casualty at the (now 'old') Westminster Hospital, London SW1...
Differentiating between sacral pressure damage and moisture lesions is not always straightforward. Fortunately, help is at hand.

This article outlines the breadth of Changing Faces’ work, our perspective on what health care for people with disfigurements should look like – and what we offer in the form of training and advice for health and social care professionals.
Granulox (Infirst Healthcare) is an innovative haemoglobin spray which improves the oxygen supply to chronic wounds through simplified diffusion, thereby promoting wound healing.

This month's selection of Tweets which caught our attention.
If you have any comments, opinions or would like to submit an article, please email, Tweet us or leave a comment on our Facebook page. We would love to hear from you.
What is your opinion on the proposed payment of £55 to GPs for every patient diagnosed with Dementia?
The EPUAP has announced the recent death of Dr. George Cherry.

According to the 2011 Census there are 200,000 young carers (under 18) in the UK; however, a BBC survey in 2010, estimated that there could be as many as 700,000.
This is Lauren's story

Love it or loath it, technology, in particular social media, is here to stay. But can it be of benefit to nurses?

SCA is excited to announce product upgrades to two of its most popular ranges, TENA Slip and TENA Comfort.
BSN has launched a new ‘Quick Guide’, Managing Chronic Oedema with a Venous Leg Ulcer. It contains practical help and advice, and is available free of charge.
Children’s allergies such as cow’s milk allergy (CMA) are on the increase. Maureen Jenkins, Director of Clinical Services at national charity, Allergy UK explains what symptoms to look out for in common allergic conditions, thereby epediting diagnosis and management.
Faecal Incontinence can effect between 1% and 10% of adults, depending on the frequency and definition faecal incontinence used. It is likely that 0.5–1.0% of adults experience regular faecal incontinence that affects their quality of life. This article gives an overview of the problem and highlights some actions that nurses can take to manage this.
Skin tears are described as traumatic wounds that result from a separation in the two principle layers of the skin, the dermis and epidermis. While the STAR (Skin Tear Audit Research) tool classification of skin tears is helpful, it was recognised that wide variations in practice occur; in an attempt to address this, the International Skin Tear Advisory Panel (ISTAP) was established. Here, Annie Clothier reviews the skin tear guidance the group produced.

This article, an entry in the Mölnlycke Health Care Scholarship and Awards, outlines a study proposal which will explore the use of a wound dressing as a prophylaxis against pressure ulcer development in patients undergoing spinal anaesthesia for an orthopaedic procedure.

One hundred years ago this month (August), the world was plunged into one of the most disastrous wound scenarios; millions of them. Wounds to bodies were devastating, but the wounds to minds, determinedly unacknowledged, almost worse. Sue Smith reflects on this dreadful time.

The principles of the NHS, based on the Beveridge Report, were to provide a comprehensive service funded by taxation, available to all and free at the time of need. Given the demands placed on the NHS today, Frank Booth ponders on the issues, and offers a personal view on how costs could be ameliorated.

He's back! Some of you may remember Brian Booth as a colomnist for Nursing Times, some of you may remember him as an excellent nurse, or a ward manager. Some of you may not know him at all. But you soon will!
As ever, Brian brings a unique slant to issues affecting nurses and by extension, patients.

Healthcare professionals may view corporate governance as a rather uninteresting subject! However, it is in fact a very straight forward concept, one that everyone involved in healthcare should be able to understand. In this article, Colin Boakes gives us an overview of corporate governance and outlines why it is important.

Patients with burns are initially treated by non-specialist clinicians and then referred to a specialist burns service. This delays definitive specialist treatment and may lead to inappropriate management of patients with burn injury. In this article, the winner of the 2014 Mölnlycke Burn Care Award, Krissie Stiles, on behalf of her team, Suzie Whiting, Karen Lambourne, Eva Daní?ková, outlines their approach to developing a regional burns care advisor network and the benefits it has realised.
Patient safety and staff training are inseparable; harms are on the whole, avoidable and happen because the basic elements of observation, risk assessment and patient management are not applied. If staff are encouraged and allowed to make small beneficial improvements to care delivery then harm to patients can be reduced significantly. This article explores how playing clinical board games can facilitate learning and skill development.

Neo-Slip is a revolutionary new product that has been designed to prevent Deep Vein Thrombosis (DVT). This anti-embolism stocking application aid is brainchild of a Registered Nurse, who as a student, had noticed health care professionals struggling to apply anti-embolism stockings.
The Lindsay Leg Club Model (LLC) was conceived as a unique partnership between the district nursing team and the local community, in which patients are empowered, through a sense of ownership to become stakeholders in their own treatment. This article gives a brief overview of the model, and concludes with a blog, written by David Foster Deputy Director of Nursing and Midwifery Advisor at the Department of Health, after his visit to Mottingham Leg Club.

During June, Viv Bennett and her colleagues at the Department of Health (DH) held a week of action Health Improvement and Health Promoting Practitioners. This involved visits to a number of clinical areas. Here, David Foster, Deputy Director of Nursing and Midwifery Advisor at the DH, has kindly agreed to share his blog with us as he reflects on his visit with Liz Alderton, a district nurse and Queen’s Nurse at the North East London NHS Foundation Trust.
District Nurse numbers continue to fall. Here, the RCN raises its concerns.

This month's selection of Tweets which caught our attention.
If you have any comments, opinions or would like to submit an article, please email, Tweet us or leave a comment on our Facebook page. We would love to hear from you.
The NMC has launched a consultation on rule changes which would enable nurses and midwives to pay their annual registration fee in installments. Would you rather?
There is a ground-swell of opinion (see RCN NI news and Booth's Opinion Piece) that patients who come to A & E as a result of abuse of drugs or alcohol, in the absence of a clinical problem, should pay a fee. Do you agree?

In issue 2, we featured Helen Mountford’s winning entry in the Mölnylcke Scholarship programme. Helen is a staff nurse at Acorns Children's Hospice. This article talks about the Acorns philosophy and approaches to care.

I have to admit that I am not always backward in coming forward with an opinion if it is an issue about which I feel passionately. Indeed, I sometimes wonder if I am an exclamation mark short of being a member of the green ink brigade!

We are giving away two Archos 70 Xenon 7" mobile tablet devices to the 500th and 700th nurse who registers on the Primary Care Nursing Review website!

On May 15th I had the honour of attending the Mall Galleries, London where Changing Faces, aided by the broadcaster and journalist, Mishal Husain, were launching their new campaign, ‘What Success Looks Like’.
Press 'read' to learn more
New research has found that the riding position of motorcyclists is a contributory factor in lower limb venous disease and the development of venous ulceration. However, according to a survey, 60 per cent of motorcyclists would not consider wearing compression hosiery which can prevent lower leg problems, despite two-in-five complaining of cramps and leg pains after riding.
The next generation of bandages may be able to tell you when a wound needs attention and in some cases, actually start the process.
Coloplast and the University of Ulster have developed and launched a new on-line resource to help specialist nurses communicate their work to others for the benefit of patients.
It's RCN Congress time again! This year, Congress will take place from the 15th - 19th June at the Liverpool Arena and Conference Centre.

Helen Mountford who is a staff nurse at the Acorns hospice in Walsall has been named as the overall winner of this year’s Wound Academy Scholarships and Awards.
Urinary catheterisation is as old as the hills, affects thousands of people a year and costs millions of pounds. And yet patients continue to suffer catheter associated urinary infections (CAUTI), or experience discomfort during the procedure or while the catheter is in situ. Add to this the fact that primary care workloads never get lighter, and it would seem obvious that this most basic of all procedures should be simple. So, refreshing one’s knowledge base can only help.
Lymphoedema is frequently misunderstood and thus mismanaged. This article, taken from the document ‘Best Practice For the Management of Lymphoedema – 2nd Edition: Surgical Intervention – A position document on surgery for lymphoedema’, outlines the causes of this disease, its classification and progression and the signs to be aware of.
The cornerstones of lymphoedema management as outlined in the literature include:
Compression bandaging plays a central role in the management of all forms of chronic oedema and lymphoedema.

Patients receiving end-of-life care are susceptible to pressure ulcers and other wounds. However, all too often, these are viewed as untreatable as it is unlikely that they will heal. In this article, Helen Mountford, the 2014 Mölnlycke Wound Academy Scholarship winner, outlines why wound care is important in paediatric end-of-life care, her work in this area to date, and what she hopes to achieve as a result of winning the Scholarship.
A substantial increase in the number of residential home patients referred to the Integrated Community Team (ICT) for pressure ulcer management highlighted the need for ongoing improvements in care standards with these homes. In response, a project was defined with the specific aim of enhancing the standard of care within RHs. This article, adapted from a poster presented at the European Wound Management conference 2014, outlines a collaborative initiative between the Tissue Viability Service, Basildon ICT, and Smith & Nephew.

In this case-study, the highly commended entry in the Molnlycke Wound Cademy Scholarship and Awards, Wendy Luke outlines the care of a patient with Chronic Obstructive Pulmonary Disease. It shows how Wendy and the team had worked together to find a suitable dressing that would both maintain the seal on her ventilation mask, and allow treatment to be applied to the small pressure ulcer on her face.
Mepitel One as a primary dressing was used as it could be removed without pain or trauma. The wound healed, and the patient continue to use the dressing prophylactically.

Continence (or rather, incontinence) was a taboo subject for many years; it became the 'butt-end' of many comedians’ jokes, living in the same realm as sexual innuendo. In this opinion piece, Frank Booth, a retired usrology nurse specialist, reflects that despiteattitudes towards this subject relaxing somewhat, community nurses still have to help and support patients living with incontinence.

Sue Smith reflects on the patients that made a lasting impression upon her during as a first year student nurse on her first stint of night duty
Picture the scene; you’ve been asked to do a presentation at a forthcoming study day. This means that someone thinks the work you are doing deserves a wider audience – yeah! But then you think, ‘If I’m standing on the stage doing the presentation, it’s assumed that I’m the one who knows more, or at least as much, as those sitting in the audience.
While the rain in Birmingham managed to dampen most things, it failed to dampen the enthusiasm of the delegates, speakers and exhibitors at the annual Association for Continence Advice (ACA) conference, held at the Hilton Birmingham Metropole hotel.
The new health and care system will deliver the ambitions set out in the Health and Social Care Act. NHS England, Public Health England, the NHS Trust Development Authority and Health Education England will take on their full range of responsibilities.
The NMC is currently revising the Code, and is seeking the views of patients, the public, nurses, midwives and other organisations or individuals who may be affected by changes to the Code.
Community nursing charity The Queen’s Nursing Institute has announced the start of a new three-year project to improve the health of people who are homeless.
In this update, we bring you news of the comings and goings of RCN NI members and RCN NI activity.
Coloplast and the University of Ulster have developed and launched a new on-line resource to help specialist nurses communicate their work to others for the benefit of patients. Specialist nurses have a wide and deep knowledge of their specialty, but have not necessarily developed the knowledge and skills to manage the demands of being a specialist nurse.
A study published in the Radiotherapy & Oncology Journal has shown that the use of Mepitel Film® dressings prevents the development of moist desquamation: painful skin ulcerations associated with breast cancer radiation therapy. The study also found that the same dressing reduced the overall severity of skin reactions such as itching and irritation by 92%.

If you have any comments, opinions or would like to submit an article on any of the topics, Email, Tweet us or leave a comment on Facebook. We would love to hear from you.
15th -19th June 2014
Arena and Convention Centre, Liverpool
30th June – 2nd July 2014
Crowne Plaza Hotel, Glasgow
29th September
The Royal Garden Hotel, 2-24 Kensington High Street, London
Tap your answer and view the results from other readers instantly.
Tap your answer and view the results from other readers instantly.
Dermatology & wound care clinical trials. If you are interested in becoming involved in this type of research we would like to make contact with you.
Mölnlycke Health Care is committed to supporting practitioners’ professional development through both formal and informal methods. One of the main tenets of this delivery framework is the Wound Academy, which supports the Scholarship and Awards programme.
The Scholarship and Awards Programme (SAAP) has been running for 12 years. During this time, the programme has supported and enabled wound care teams, experienced practitioners and novice practitoners to realise projects within their organisation, and facilitated professional development through the support framework provided in the year following the Scholarship.
No, we’re not being sexist! Just that even today most nurses are female, so it’s easier than writing he/she, him/her etc…

Welcome to the inaugural issue of Primary Care Nursing Review (PCNR)! PCNR is a bi-monthly journal aimed at nurses and other health professionals working in all areas of primary care across the UK.
You may be wondering why on earth we’ve decided to launch another journal – and you wouldn’t be alone in thinking that, it’s crossed our minds once or twice too! However, this is something very different. There is a plethora of worthy nursing and health titles about all aspects of care, but often these are hard work to read and only focus on a limited number of subjects which may not truly reflect the complexity of healthcare issues that arise in your day to day role. How many of you intend to read your favourite journal, but end up just staring at the pile accumulating on the floor thinking ‘I must get around to reading those…’?

The number of District Nurses in England in May 2010 was 7,813; there are now 2,020 fewer.

The developers of Surgihoney have postulated that given the doubts raised about the research methodologies used to demonstrate the effects of manuka honey, clinicians should stop using it and its derivatives.
The Government is consulting on making “wilful neglect” of patients a criminal offence in England. Any health professional successfully prosecuted could face up to five years imprisonment and/or £5,000 in fines, and their employing organisation receiving financial penalties.
The Erasmus Medical Centre, Department of Dermatology, Rotterdam and the Dutch Institute of Allied Health Care, Amersfoort, both in The Netherlands, are currently embarking on the development of International Classification of Functioning, Disability and Health (ICF) Core Sets for Lymphoedema.
Study shows yoghurt consumption reduces the risk of type 2 diabetes

Although honey has been used for wound/infection management for millennia, it was only ‘rediscovered’ as a topical antibacterial agent in 1892. Ian Staples explores the benefits of this remarkable treatment.
Alan Jackson looks at the problem of healthcare and obesity and asks how nurses can find the time to help people lose weight when the overwhelming emphasis is on essential care for their primary condition.
In light of literature which suggests many patients are unable or unwilling to follow self-care activities, Annemarie Brown looks at how post-ulcer healing interventions should focus on minimising recurrence and enabling patients to adapt their lives to living with chronic venous ulceration (CVLU).
Community nurses play a crucial role in the primary health care team, particularly for people with dementia who may be living at home but find it harder to get out of the house for health care appointments. As well as providing direct care, community nurses also have a teaching role, working with patients to enable them to care for themselves or educating family members. Community nurses play a vital role in keeping hospital admissions and readmissions to a minimum and ensuring that patients can return to their own homes as soon as possible.

Sue Smith trained as a State Registered Nurse in the days of re-sterilising bandages and equipment, bottle/bedpan rounds and cooking milk puddings for ‘the gastric patients...’ However, a life-time both in both community nursing and nursing journalism, has given her great insight into the needs of patients.
Today, we are continually being asked to prove our worth, demonstrate effectiveness, and present outcomes which may or may not determine payment. However, at times it’s like we are living in the middle of Heisenberg’s uncertainty principle; the more precisely you measure one quantity, the less precisely you can know another associated quantity; for example, both healing (a) and well-being (b) may be quantities we measure as outcome indicators in wound management. However, if we are being asked to focus on measure (a), which is a likely request from a commissioner, are we in danger of being unable to measure (b), which is probably more important to the patient?
So in order to remove any uncertainty, community nurses must face such challenges head-on and work with commissioners to ensure a patient-centred outcome rather than a resource-centred one. In this article, we look at the role of Clinical Commissioning Groups and hear from both the Chief Operating Officer and the Executive Nurse.
The NHS reforms brought about by the Health and Social Care Act 2012 are being embedded, but the pace and complexity of nursing work continues. In this article, Dr David Foster, Deputy Director of Nursing and Midwifery Advisor, Department of Health, outlines how he and his colleagues support the work you are doing.
The Queen’s Nursing Institute (QNI) is a charity that traces its origins to 1887. Initially established to co-ordinate and set national standards for District Nurse training across the country, it now has a much wider remit.
Here, Crystal Oldman, Chief Executive, talks to Deborah Glover about the history of the QNI, their work today and share some thoughts on the future.
The NMC is currently consulting on their proposed model of revalidation, the process by which registered nurses and midwives are required to demonstrate to the NMC that they remain fit to practise. It promotes greater professionalism among nurses and midwives and also improves the quality of care that patients receive by encouraging reflection on nurses’ and midwives’ practice against the revised Code.
The content and format of the NMC Code will be revised, and supporting guidance specific to revalidation will be developed.
Community nurses, midwives and health visitors serve the population of more than 3 million people in Wales. They meet the health and nursing needs of all age groups and in all locations outside hospital environments such as at home, schools, surgeries, clinics and care homes. They are central to the Government’s aim to reduce the number of unnecessary admissions to hospital and increase early discharges from hospital. People needing community-based support can be sicker or have more complex needs than ever before.
The RCN has submitted its response to a DHSSPS consultation on a community resuscitation strategy for Northern Ireland. The strategy aims significantly to increase the number of people with CPR skills in order to provide assistance to people who suffer an out-of-hospital cardiac arrest, thus increasing their chances of survival. In its response, the RCN welcomes the draft strategy but makes a number of suggestions for strengthening it, particularly in respect of securing ownership within communities.
Nursing leader backs Children and Young People Bill amendment on health visitors.
On the 7th January, MSPs debated whether health visitors should be the ‘Named Person’, i.e., the individual who provides first line support and advice for children aged 0 – five. The RCN Scotland is backing an amendment to the Children and Young People Bill to explicitly state that the health visitor should be the Named Person for this age group, following on from the midwife in the very first days of a baby’s life.

The European Oncology Nursing Society is a pan-European organisation dedicated to the support and development of cancer nurses. Through individual members and national societies we engage in projects to help nurses develop their skills, network with each other, and raise the profile of cancer nursing across Europe.

Within three short months of their daughter Florence’s birth, Judith and Chris Parsons’ world was turned upside down. Eczema was diagnosed and standard creams and emollients for symptom control prescribed.
Currently there is no cure for these distressing and often disabling conditions, and service provision for affected patients appears to be inconsistent. Current recommended treatment is aimed at decreasing swelling, pain and discomfort, using a combination of massage and compression garments known as Complex Decongestive Therapy (CDT), or Decongestive Lymphatic Therapy (DLT).

If you have any comments, opinions or would like to submit an article on any of the topics, Email, Tweet us or leave a comment on Facebook. We would love to hear from you.
1st & 2nd April 2014
York University, York, UK
Wound Care Alliance
11th April
Swansea, UK
NMC
1st May 2014
Hallam Conference Centre, London
8th & 9th May
Birmingham Hilton Metropole, Birmingham
9th & 10th May 2014
Scarman House, University of Warwick
14 -16th May
Madrid, Spain
15th -19th June 2014
Arena and Convention Centre, Liverpool
30th June – 2nd July 2014
Crowne Plaza Hotel, Glasgow
An introduction to Lipoedema Ladies by Michelle Ellis
I found out I had Lipoedema when it was too late. I was 30 and had already developed Lipo-Lymphoedema. I am lucky I was diagnosed at all: there are 3.2 million women in the UK with undiagnosed Lipoedema.
This series takes an educated guess as to what a nurse would do in any given circumstance.
Your contributions are welcome! Send to deborah@pcnr.co.uk
Primary Care Nursing Review is a new digital journal which has been created for users of mobile devices such as smart-phones or tablets. Of course, you can also view the journal content from your desktop screen, but we know that many of you are more likely to be on the move and have your Wi-Fi, 3G, or even 4G-enabled device close by, so we made something specifically for you.
A brief guide to help you navigate the journal. You'll only need to look at this once because it's intuitive and user friendly!